Lipopolysaccharide-Induced Acute Inflammation in Mouse Lung
Robert Xiaxuan Lao
Mentor: Professor Hartmut Grasemann, MD
1.0 Abstract
1.1 Rationale
Lipopolysaccharides (LPS) from gram-negative bacteria have the ability to induce immune responses in humans. The presence of cells, such as macrophages and neutrophils, as well as production of nitric oxide (NO) is increased in such circumstances. We studied the effects that LPS has on pulmonary function in mice, to serve as a basis for future implementations of LPS for medical treatment of induced inflammation in human beings.
1.2 Method
Mice underwent tracheal instillation of LPS. Lungs were harvested on the third day post instillation. Cell analysis was performed by extracting broncho-alveolar lavage (BAL) solution and then performing hemacolor staining. Inducible nitric oxide synthase (iNOS) expression was quantified through real-time or quantitative polymerase chain reaction (qPCR).
1.3 Results
In LPS infected mouse lung, the presence of neutrophil (92%±4% vs. 2%±3%, p<0.01) increased significantly compared to that of non-infected mouse lung. In addition, after normalization for the housekeeping gene hypoxanthine-guanine phosphoribosyltransferase (Hprt), there was a significant increase (900±300 fold, p<0.0005) in the expression iNOS in LPS infected mouse lung compared with non-infected controls.
1.4 Conclusions
LPS induces acute inflammation in mouse lung. It can induce significant increases in the production of neutrophils as well as increase iNOS expression, via NO or oxidant peroxynitrite (ONOO-) in the pathogenesis of LPS induced inflammation.
2.0 Introduction
The airways and lungs are frequent targets of infections such as acute bronchitis or pneumonia. Acute inflammation caused by bacteria can promote the mobilization of large white blood cells (phagocytes) to an injured or infected area in order to kill extracellular bacteria. One well-established stimulus commonly used to recapitulate clinical aspects of lung bacterial inflammatory infection is the bacterial endotoxin – lipopolysaccharide (LPS). LPS from many gram-negative bacteria species can initiate acute inflammatory responses in mammals and can range from pyrexia to gram-negative septic shock [1]. LPS elicits multiple pathological effects in human beings. For example, LPS can activate alveolar macrophages and bring about neutrophil infiltration resulting in damage of the lung tissue including the air–blood barrier [2]. In addition, LPS can provoke acute lung injury (ALI) and the acute respiratory distress syndrome (ARDS). Recent studies have also explored new respiratory defense mechanisms, such as neutrophil extracellular traps (NETs), by instilling LPS into the respiratory tract and lungs [3].
LPS are large molecules consisting of a lipid and a polysaccharide. These molecules are found in the outer membrane of Gram-negative bacteria. Acute exposure to LPS provokes the innate immune system, initiating a cascade of inflammatory cell influx which leads to an increase in cytokine release and lung injury [4][5].
The human innate immune system is comprised of various immune cells such as neutrophils and macrophages. Both cells can engulf and destroy pathogens, such as bacteria, through phagocytosis. Neutrophils are the most abundant (40% to 75%) type of white blood cells in mammals and form an essential part of the innate immune system. They are formed from stem cells in the bone marrow and are short-lived and highly motile. Macrophages are found in essentially all tissues, where they patrol for potential pathogens by amoeboid movement. They play a critical role in non-specific defense and also help initiate specific defense mechanisms.
When neutrophils and macrophages are activated, they can express a type of nitric oxide synthase (NOS) called inducible nitric oxide synthase (iNOS). NOS is the enzyme that catalyzes the production of nitric oxide (NO) by metabolically converting L-arginine into L-citrulline. There are three distinct isoforms of NOS which differ both in their structure and function. Endothelial NOS (eNOS) and neuronal NOS (nNOS) are generally referred to as constitutively expressed, calcium-dependent enzymes. iNOS is calcium-independent and expressed at high levels only after induction by certain cytokines or other inflammatory agents. Activated iNOS produces large amounts of NO [6]. The iNOS product is a free radical with an unpaired electron, which is biologically cytotoxic and is able to directly kill invading bacteria.
In this study, LPS was instilled into mouse trachea and lungs to observe the acute inflammatory cell influx in the respiratory system and the change in iNOS expression. The purpose of this study is to strive to be a model for future research into medical treatments of LPS induced inflammation responses in humans.
3.0 Method
3.1 Mice Model
Ten BALB/c mice were used for this study. Five BALB/c mice were injected with 5µg of LPS in 50µl PBS on the first day. Five non-LPS injected BALB/c mice were used as the control group and were instead injected with 50µl PBS. For instillation of LPS into the trachea, mice were first anaesthetized with ketamine (150 mg/kg; Bioniche Animal Health, Toronto, ON, Canada) and xylazine (5mg/kg; Bioniche Animal Health, Toronto, ON, Canada) solution, which were injected intraperitoneally. Once the mice were anaesthetized (without pedal or ocular reflex), each mouse was instilled intratracheally with its respective inoculums for each group. The mice were held on a restraining board at the 45? diagonal position. A 24 GA BD Angiocath IV catheter was inserted into trachea through the pharynx and between vocal cords for injection of the inoculums to the airways. Each mouse was instilled with 5µg LPS in 50µl PBS volume or 50 µl PBS. The body weight of each mouse was monitored: one-day pre-injection and every day post-infection for 2 days. After 2 days, the mice were sacrificed with ketamine and xylazine injection. Then broncho-alveolar lavage (BAL) was performed. Lung tissues were harvested and stored in liquid nitrogen immediately afterward. The tissues were then stored at -80ºC until further use. The animal care facility’s ethics committee approved all protocols involving mice and experiments were conducted in accordance with the guidelines of the Canadian Council for Animal Care. All buffer salts and reagents were obtained from Sigma-Aldrich unless otherwise stated.
3.2 BAL and Cell Analysis
After administration of ketamine and xylazine on day 2 with the intent of sacrificing the mice, a tracheotomy was then performed for each mouse. Tissue was dissected from neck to expose trachea and small incisions were made in the trachea to allow passage of 18-gauge lavage tube. Then the tube was passed into the trachea and stabilized by using surgical sutures. BAL was performed with 1 ml PBS per wash using 1ml syringes. 2 washes were performed for each mouse (I think you should use less “with”). BAL fluid was then centrifuged for 10 min at 400g to pellet cells. The cells were then resuspended in PBS buffer. Total cell count was performed by manual counting using a hemocytometer, and cytospin preparations were made for differential cell counts. For differential cell count, cells were stained with a Hemacolor histology staining kit (EMD Chemicals, Gibbstown, NJ). Cell types were quantified from randomly taken images of cytospin preparations. At least 500 cells were counted for each condition for analysis.
3.3 RNA Isolation
Total RNA was extracted from mouse lung tissue samples. Lung tissue samples were homogenized in TRI reagent (TRI Reagent, ThermoFisher Scientific) and total RNA was extracted according to the manufacturer’s protocol. A brief overview of the protocol: the homogenate was centrifuged at 12,000 g for 10 minutes. The supernatant was collected and added with 100µl BCP (3-Benzidino-6-(4-chlorophenyl)pyridazine) per 1 ml of TRI reagent solution. Then the solution was shaken vigorously for 15 seconds and incubated at room temperature for 10 minutes. The homogenate with BCP was then centrifuged at 12,000g for 10 minutes at 4?C and the aqueous phase was transferred to a fresh tube. The RNA pellet was recovered by precipitating RNA with 500 µl isopropanol per 1 ml of TRI reagent solution and centrifuged at 12,000g for 10 minutes. The recovered RNA pellet was washed with 75% ethanol. Finally, the RNA pellet was dissolved in the nuclease-free water. RNA quantity, purity were checked by spectrophotometry. The A260/ A280 values in all RNA samples were between 1.8 – 2.1. RNA concentration was determined by the OD reading at 260nm as given by the following conversion: an A260 of 1.0 is equivalent to 40 µg/mL of RNA. RNA integrity was checked by running the RNA on a 1% standard agarose gel. 28S and 18S ribosomal RNA bands were clearly visible in all RNA samples.
3.4 Reverse transcription
Total RNA was reverse transcribed using Superscript III first-strand synthesis supermix for qPCR (Invitrogen Canada). The First-Strand complementary DNA (cDNA) was synthesized according to the manufacturer’s protocol. A brief overview of the protocol: a 20 ?L cDNA reaction volume was prepared by mixing 2X reaction mix 10µl, reverse transcription enzyme mix 2 µl, RNA 1 µg and DEPC water to 20ul. Then, reaction mix was incubated at 25°C for 10 minutes then 50°C for 30 minutes. The reaction was terminated at 85°C at 5 minutes, and then chilled on ice. Finally, the remaining RNA was removed by adding 1µl (2U) of E. Coli RNase H and incubated at 37°C for 20 minutes. The cDNA samples were then stored at -20°C until further use.
3.5 Real Time Polymerase Chain Reaction (qPCR)
Quantitative real time PCR amplification was performed with primers in combination with SYBR green (Power SYBR Green PCR master mix, Applied Biosystems) on an Applied Biosystems 7900HT Real Time PCR System. Primer sets for sense (S) and antisense (AS) amplifications for the following genes were used: for inducible nitric oxide synthase (iNOS), 5’- GCCCCTGGAAGTTTCTCTTC -3’ (S) and 5’- GTCGATGTCACATGCAGCTT -3’ (AS) and as endogenous control, for hypoxanthine guanine phosphoribosyltransferase (Hprt) 5’- TGATCAGTCAACGGGGGACA -3’(S) and 5’- TCCAACACTTCGAGAGGTCC -3’(AS).
All PCR protocols included a 10-minute polymerase activation step followed by 40 cycles consisting of a 95°C denaturation for 15 seconds, annealing at 60°C for 1 min, and an elongation step at 72°C for 1 minute. Dissociation curve and agarose gel electrophoresis were used to examine each sample for purity and specificity. The amount of target gene and endogenous control was determined from the standard curve that was constructed using appropriate dilution series. In brief, relative fold changes in target gene expression were calculated from the efficiency of the qPCR reaction and the crossing point deviation between samples from LPS infected mice and wild-type littermate controls, and determined by normalization to expression of the reference gene Hprt, as previously described [7].
3.6 Statistical analysis
All final values are expressed as average ± standard deviation. For comparison between two groups, the student’s t-test was used where p values were set and needed to be at 0.05, 0.01, 0.001 or less in order to be statistically significant. All statistical analysis was performed using the appropriate respective functions in Microsoft Excel.
4.0 Results
It was observed that the body weight of control mice increased slightly throughout the experiment duration, which was expected. However, the body weight of LPS infected mice decreased significantly in the two days after injection as shown in Figure 1. On post-infection day 1, mice lost (4.3±0.8)% of their body weight. On post-infection day 2, they lost (6±2)% of their original body weight.
Fig 1. Shows the weight change of control and LPS injected groups of mice during the experiment from Day 0 to Day 2 with respect to Day -1 (before experiment) as a percentage. As seen in the figure, the weight of the LPS injected group of mice significantly decreased throughout the time of the experiment compared to the stable weight of the control group of mice.
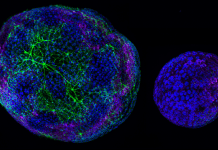
Seen in Figure 2, cell samples taken from control mice have a composition of almost entirely macrophages with little to no neutrophils. Macrophages are large cells usually with one large visible nucleus. However, cell samples taken through BAL of LPS treated mice have a composition of mostly neutrophils along with some macrophages. Neutrophils are small multi-lobed cell connected by thin strands of nuclear material.
4.2 Cell Differentiation in Control vs BAL of LPS Injected Mouse
Fig 2. Comparison of cell slides. The left slide was taken through BAL from the control group and the right slide taken through BAL from the LPS injected mice group. Scale bar measures 50 µm across. As seen the BAL from the LPS injected mice group contains significantly more neutrophils compared to none visible in the BAL from control.
These results are also represented numerically in Figure 3 demonstrating a significant increase in the number of neutrophils present in LPS injected mice cell samples.
4.3 Total Cell Count and Cell Differentiation in BAL of LPS Injected Mouse
Fig 3. Shows the number of cells, macrophages and neutrophils per mL in both the samples taken from the control group and the LPS injected group of mice as well as their t-test results respectively. The percentage difference in composition of BAL from control and LPS injected mice groups can be seen. Seemingly a percentage majority switch between Macrophages and Neutrophils between the two groups.
Figure 4 shows the amplification plots for two different genes – iNOS (on the right) and Hprt (on the left) in all mouse lung samples. Rn is the fluorescence of the reporter dye divided by the fluorescence of a passive reference dye; in this study, Rn is the SYBR Green signal normalized to the fluorescence signal of ROX™ [8]. ?Rn is Rn subtract the baseline. Figure 4 has the ?Rn plotted against the PCR cycle number. A relative measure of the concentration of target in the qPCR reaction can be indicated by Ct (threshold cycle), which is the intersection between an amplification curve and the threshold line. In the amplification plot of iNOS (right), there are two groups of amplification curves. The Ct data in one group of mice was located between 24~25, which were from LPS-infection mice. However, the Ct data in the other group of mice was located between 33~35, which were from PBS control mice. So the plot shows a huge difference of iNOS concentration between LPS injection mice and control mice. But in the amplification plot of housekeeping gene Hprt, there is no difference in the amplification curves of all detected mice, which means LPS induced iNOS expression specifically. Fig 3. Shows the number of cells, macrophages and neutrophils per mL in both the samples taken from the control group and the LPS injected group of mice as well as their t-test results respectively. The percentage difference in composition of BAL from control and LPS injected mice groups can be seen. Seemingly a percentage majority switch between Macrophages and Neutrophils between the two groups.
4.4 Amplification Plot of Hprt versus iNOS in LPS Injected Mouse
Fig 4. Shows the amplification plots from qPCR of a housekeeping gene Hprt, shown on the left, and iNOS, shown on the right. While in the control group, there is one clear peak in the amplification plot, in the LPS injected group, two clear peaks can be visualized in the amplification curves.
As shown in Figure 5, there is a significant 900±300 fold change increase in iNOS expression in LPS injected mice lung compared to control mice after normalization to Hprt.
Fig 5. Shows the fold changes of iNOS mRNA expression in comparison to a housekeeping gene in LPS injected mouse lung with respect to the control mouse lung calculated using the standard curve method.
5.0 Discussion
Our result demonstrates that without LPS treatment, the BAL cells from control mice are mainly composed of macrophages with little to no measureable composition of neutrophils. The lavage fluid contained (96±3)% macrophages. However, 2 days after inducing inflammation of the trachea and lungs with LPS , neutrophils are the dominant cell type. The lavage fluid taken from the LPS-injected mice contained (92±4)% neutrophils. Both neutrophils and macrophages are the first-line innate immune defense cells that are able to capture and kill microbial pathogens. Alveolar macrophages (AMs) and neutrophils are both phagocytic cells that can clean off particles such as bacteria. Furthermore, activated neutrophils can generate DNA-based neutrophil extracellular traps (NETs) to trap and kill various microbial [3][9].
Under normal circumstance, in the pulmonary immune system, alveolar macrophages act as the first line of defense against inhaled particulates and pathogens, and they play an essential role in both the initiation and orchestration of inflammatory responses. Thus, AMs are not only excellent phagocytes capable of removing particulates and pathogens from the airway, but they can also promote innate and adaptive immune responses [10]. Even ambient air contains the bacterial endotoxin LPS. Every time we take a breath, we have potential to inhale LPS in to our lungs which may cause damage to the lung based on a pre-existing disease or condition in the body. In other words, we are involuntary primed by endotoxin [6][11]. Therefore, the AMs have a critical role in the host’s lung defense. AMs contribute to innate immunity in the lung by virtue of their ability to migrate, undergo phagocytosis, kill microorganisms, and recruit and activate other inflammatory cells. Macrophages also provide important links between innate and adaptive immunity, by Toll-like receptor mediated pathogen recognition that results in a release of cytokine capable of reprogramming other innate and adaptive immune responses [12].
After intratracheal exposure to low doses (5µg) of LPS for 48 hours, LPS was able to provoke the innate immune system to react by releasing fighter cells such as AM, initiating a cascade of inflammatory cell and neutrophils to influx into the lungs and trachea. The present study demonstrates that intratracheal LPS administration induces neutrophil recruitment into airway and lung of mice. In two days, there was a significant neutrophil influx into the alveolar space, forming a predominantly neutrophil filled environment in the BAL fluid. This occurred because of the ability of LPS to serve as a ligand for Toll-like receptor 4 (TLR-4), a protein in humans responsible in the activation of the innate immune system when stimulated by LPS. Subsequently, this activated the transcription of the major neutrophil chemokine interleukin 8 (IL-8) in humans, or KC and MIP-2 (mouse homologs of IL-8) in mice [13]. Besides, LPS, one of the major pro-inflammatory constituents of the cell walls of gram-negative bacteria, induces AMs to express interleukin-1 (IL-1) and tumor necrosis factor (TNF). IL-1 and TNF are important pro-inflammatory cytokines and known to recruit neutrophils and mononuclear inflammatory cells into the alveolar space [14].
Intratracheal instillation of LPS resulted in a significant increase in mRNA expression of the inducible isoform of NOS. In this study, only iNOS mRNA was particularly prominent among three isoforms of NOS. The mRNA of the other two isoforms were not increased (results not shown), which indicated this isoform (iNOS) as a key enzyme for NO production in the infection. Thus, these results are in agreement with current studies [6]. eNOS and nNOS are generally calcium-dependent enzymes that produce low levels of NO as a cell signaling molecule. iNOS is involved in immune response, binds calmodulin at physiologically relevant concentrations, and produces NO as an immune defense mechanism. When LPS enters the trachea, it can make cells such as macrophage, bronchial epithelium cells and neutrophils produce iNOS. Our observations suggest that at the peak of acute inflammation, most NOS activity could be attributed to iNOS in activated neutrophils. The inducible isoform iNOS produces large amounts of NO as a defense mechanism to kill the invading bacteria. Thus, iNOS and respectively NO, are very important in the human body’s ability to defend against pathogen [15][16].
However, besides synthesizing NO, NOS are able to catalyze superoxide anion (O2-) formation especially in the absence of L-arginine. NOS are bi-domain enzymes that consist of a C-terminal (reductase) and N-terminal (oxygenase). In iNOS, NO production occurs at the reductase domain while O2- formation happens at the reductase domain [17]. In absence of L-arginine, iNOS generates O2- leading to the formation of potent oxidant peroxynitrite (ONOO-) [18]. For iNOS, in the presence of sufficient L-arginine, O2- and NO production may occur simultaneously at the reductase and oxygenase domains, respectively, which can interact to form ONOO- [17]. With relatively high L-arginine levels in cytosol (200–800 µM), under normal physiological conditions, O2- generation would rarely occur.
Production of iNOS mediated O2- and ONOO- can lead to increases in antibacterial activity but can also lead to increased tissue damage to the host because both NO and ONOO- are cytotoxic. Thus, iNOS, derived O2- and ONOO, are controlled by the availability of L-arginine to NOS. Intracellular L-arginine concentration may be regulated by two distinct mechanisms: increased arginase activity, competing with iNOS for L-arginine, and specific cationic amino acid transporters (CATs) for L-arginine transport into the NO producing cells [19]. In circumstances such as cystic fibrosis where arginase activity is increased in the lung, the iNOS induced NO production can be impaired which may be relevant in the pathogenesis of CF airway disease [16][20]. Since L-arginine is an essential substrate in forming iNOS and NO, current studies are looking for ways to increase L-arginine availability to improve NO production to enhance anti-bacteria and pulmonary function in conditions with inadequate NO formation [21].
In summary, our study indicated that low dose LPS (5µg) can induce acute inflammation in mouse lung. As well, it can induce significant increases in production of neutrophils, iNOS expression. Therefore, with sufficient amounts of L-arginine, LPS induced NO production can be used to defend against pathogens.
6.0 References
- Schletter J, Heine H, Ulmer AJ, Rietschel ET. (1995) Molecular mechanisms of endotoxin activity. Archives of Microbiology, 164(6), 383–389.
- Blackwell, T.S., Lancaster, L.H., Blackwell, T.R., Venkatakrishnan, A., and John, W.C., (1999). T.Chemotactic Gradients Predict Neutrophilic Alveolitis in Endotoxin-treated Rats, American Journal of Respiratory and Critical Care Medicine, 159(5), 1644-1652.
- Douda, D., Jackson, R., Grasemann, H., & Palaniyar, N. (2011). Innate Immune Collectin Surfactant Protein D Simultaneously Binds Both Neutrophil Extracellular Traps and Carbohydrate Ligands and Promotes Bacterial Trapping. The Journal of Immunology, 187(4), 1856-1865.
- Hakansson, H.F., Smailagic, A., Brunmark, C., Miller-Larsson, A., Lal, H. (2012). Altered lunf function relates to inflammation in an acute LPS mouse model. Pulmonary Pharmacology & Therapeutics, 25(5), 399-406.
- Kabir, K., Gelinas, J.P., Chen, M., Chen, D., Zhang, D., Luo, X., et al. (2002). Characterization of a murine model of endotoxin-induced acute lung injury. Shock, 17 (4), 300–330.
- Andrew, P., & Mayer, B. (1999). Enzymatic function of nitric oxide synthases. Cardiovascular Research, 43(3), 521-531.
- Pfaffl M.W. (2001) A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res.29(45)
- Heid, C.A., Stevens, J., Livak, K.J., et al. (1996). Real time quantitative PCR. Genome Res., 6(10), 986-994.
- Reutershan, J., Basit, A., Galkina, E. and Ley, K. (2005). Sequential recruitment of neutrophils into lung and bronchoalveolar lavage fluid in LPS-induced acute lung injury. AJP: Lung Cellular and Molecular Physiology, 289(5), 807-815.
- Katsura, Y., Harada, N., Harada, S., Ishimori, A., Makino, F., Ito, J., Kamachi, F., Okumura, K., Akiba, H., Atsuta, R., and Takahashi, K. (2015). Characteristics of alveolar macrophages from murine models of OVA-induced allergic airway inflammation and LPS-induced acute airway inflammation. Exp Lung Res Experimental Lung Research, 1-13
- Inoue, H., Shimada, A., Kaewamatawong, T., Naota, M., Morita, T., Ohta, Y., Inoue, K., Takano, H. (2008) Ultrastructural changes of the air–blood barrier in mice after intratracheal instillation of lipopolysaccharide and ultrafine carbon black particles. Experimental and Toxicologic Pathology, 61(1), 51-58.
- Jab?o?ska, E., Pu?ewska, W., Marci?czyk, M., Grabowska, Z., Jab?o?ski, J. (2005). iNOS production by neutrophils in cancer patients. Arch Immunol Ther Exp (Warsz), 53(53), 175–179
- Chang, S., Linderholm, A., and Harper, R. (2015) DUOX-Mediated Signaling Is Not Required for LPS Induced Neutrophilic Response in the Airways. PLoS ONE, 10(7): e0131810.
- Ulich, T., Yi, E., Yin, S., Smith, C., & Remick, D. (1991). Intratracheal Administration of Endotoxin and Cytokines. Clinical Immunology and Immunopathology, 138(6), 137-140.
- Mehl, A., Ghorbani, P., Douda, D., Huang, H., Palaniyar, N., et al. (2014) Effect of Arginase Inhibition on Pulmonary L-Arginine Metabolism in Murine. PLoS ONE, 9(3), e90232.
- Jaecklin, T., Duerr, J., Huang, H., Rafii, M., Bear, C., Ratjen, F., Kavanagh, B.P., Mall, M.A., and Grasemann, H. (2014). Lung arginase expression and activity is increased in cystic fibrosis mouse models. Journal of Applied Physiology, 117(3), 284-288.
- Xia, Y., Roman, L.J., Master, B.S.S., and Zweier, J.L. (1998). Inducible Nitric-oxide Synthase Generates Superoxide from the Reductase Domain. The Journal of Biological Chemistry, 273(36), 22635-22639
- Xia, Y., and Zweier, J.L. (1997). Superoxide and peroxynitrite generation from inducible nitric oxide synthase in macrophages. Proc. Natl. Acad. Sci. USA, 94(13), 6954-6958
- Maarsingh, H., Bossenga, B.E., Bos, I.S.T., Volders, H.H., Zaagsma, J., and Merus, H. (2009). L-Arginine deficiency causes airway hyperresponsiveness after the late asthmatic reaction. Eur Respir J, 34(1), 191-199
- Grasemann, H., Schwiertz, R., Matthiesen, S., Racke, K., and Ratjen, F. (2005). Increased arginase activity in cystic fibrosis airways. Am J Respir Crit Care Med, 172(12), 1523-8.
- Grasemann, H., Kurtz, F., Ratjen, F. (2006). Inhaled L-arginine improves exhaled nitric oxide and pulmonary function in patients with cystic fibrosis. Am J Respir Crit Care Med, 174(2), 208-212.