Abstract
Attention-deficit/hyperactivity disorder (ADHD) involves persistent difficulties with attention and self-regulation that can interfere with daily functioning, and adolescents’ social media habits are often discussed in that context. While prior research links general social media use to attention-related outcomes, Instagram-specific evidence remains limited. In this cross-sectional pilot study, we tested whether problematic Instagram use is associated with inattentive ADHD symptom endorsement and with performance on brief timed cognitive tasks in female adolescents and young adults. Thirteen participants aged 15-22 completed the Instagram Addiction Scale (IAS) and the inattentive items from a DSM-5 ADHD checklist. They also completed timed tasks assessing pattern recognition, spatial reasoning, and recall. Scores were combined into an overall cognitive performance index. Analyses were exploratory and included multiple-comparison adjustments for correlational tests. In unadjusted analyses, IAS scores correlated positively with inattentive symptom scores, and inattentive symptom scores correlated negatively with overall cognitive performance. IAS scores also correlated negatively with cognitive performance. However, after multiple-comparison adjustment (FDR-BH and Bonferroni), none of the correlations met q < 0.05; accordingly, effect sizes should be treated as preliminary and hypothesis-generating. Future work should incorporate validated neurocognitive batteries and objective usage measures and should test temporal ordering using longitudinal or experimental designs.
Keywords: Instagram Addiction, ADHD Inattentive Symptoms, Social Media, Cognitive Performance, Digital Media
Introduction
Attention-deficit/hyperactivity disorder (ADHD) is a neurodevelopmental condition characterized by persistent inattention and/or hyperactivity-impulsivity that interfere with functioning or development1. Across development, hyperactive-impulsive symptoms often become less overt, whereas inattentive symptoms and executive-function difficulties may persist into adolescence and young adulthood, shifting impairment toward academic demands, organization, and self-regulation2.
In females, ADHD is more likely to present with predominantly inattentive and internalizing features (e.g., quiet distractibility, anxiety), and symptoms may be masked by compensatory strategies, contributing to later recognition and underdiagnosis compared with males3,4. Given that inattention is closely tied to academic performance and everyday self-regulation, understanding factors that co-occur with inattentive symptoms in adolescents and young adults is an important research priority.
At the same time, social networking sites (SNSs) are widely used by adolescents and young adults5. Problematic SNS usage—often described as addiction-like patterns such as preoccupation, difficulty reducing use, and functional impairment—has been documented and is increasingly studied in relation to psychosocial and attention-related outcomes6. These behaviors can resemble everyday manifestations of inattention, such as frequent distraction, task postponement, and difficulty sustaining focus. However, whether they reflect clinical symptoms, amplify existing vulnerabilities, or merely share superficial similarities remains unclear6. This motivates a study that distinguishes clinical symptom measures from platform-use behaviors.
One pivotal longitudinal study followed adolescents aged 15-16 years who did not meet the ADHD symptom threshold at baseline (N = 2,587) and found that more frequent engagement in a broader set of modern digital media activities predicted higher odds of later ADHD symptom endorsement over a 24-month follow-up7. Importantly, directionality may depend on the type of use. In a three-wave study of Dutch adolescents (N = 543), addiction-like social media use problems—but not social media use intensity—predicted increases in ADHD symptoms over time, supporting the idea that problematic use is more relevant than time spent alone8. Together, these studies are consistent with a dynamic relationship between digital media behaviors and attention-related outcomes. However, they do not resolve whether platform use precedes symptom changes, whether pre-existing symptoms predict later problematic use, or whether both processes operate simultaneously under shared third factors (e.g., sleep, stress, academic pressure)9,10. Importantly, most prior works have focused on social media broadly rather than on Instagram-specific use patterns.
Instagram may be particularly relevant because several design features can promote rapid, repeated attentional shifts. Instagram includes features such as algorithmically curated feeds, short-form videos, bite-sized content, and real-time updates through Story, which may encourage repeated checking and switching. Unpredictable social feedback, such as likes, notifications, and messages, may reinforce habitual checking behaviors11. These mechanisms are hypothesized to increase attentional switching costs and working-memory load during multitasking, which could relate to perceived inattention in daily life12,13. However, Instagram-specific studies are limited, and a clearer measurement of how problematic Instagram use relates to inattention symptoms is needed.
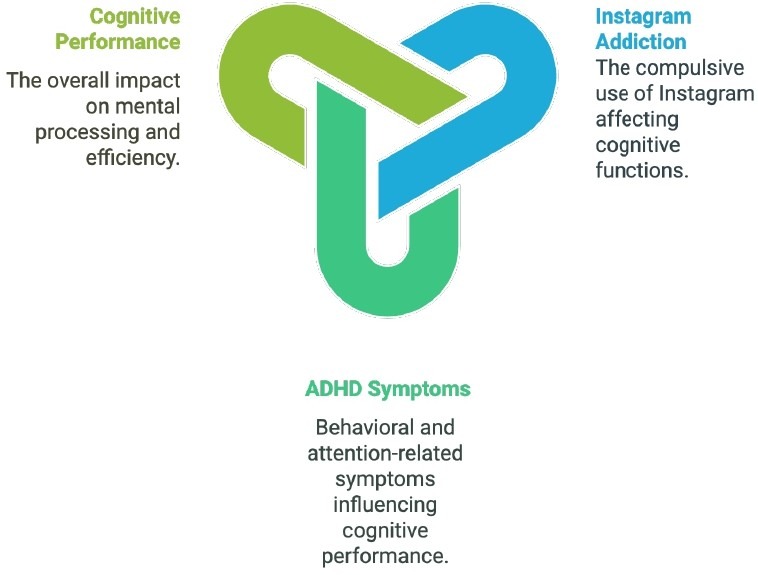
In addition to self-reported symptoms, cognitive performance is relevant because ADHD is commonly associated with variability in attentional control and executive functioning14,15. In this study, cognitive performance is operationalized as performance on brief timed tasks assessing pattern recognition, spatial reasoning, and recall. Together, these index multiple attention-relevant processes, including sustained attention and perceptual speed, executive control, and working memory (Figure 1). Mapping these tasks to attention-related domains provides construct-level motivation for examining whether problematic Instagram use and inattentive symptoms are associated not only at the symptom level but also in objective task performance.
Here, we examine associations among problematic Instagram use, inattentive ADHD symptoms, and cognitive task performance in a sample of female adolescents and young adults. Problematic Instagram use is measured using the Instagram Addiction Scale (IAS), inattentive symptoms are assessed using the inattentive items of a DSM-5 ADHD symptom checklist, and cognitive performance is summarized using a composite index derived from timed tasks. Consistent with the exploratory nature of a small-sample cross-sectional design, we seek to address two key questions: (1) Are IAS scores associated with inattentive symptom scores? (2) Are IAS scores and inattentive symptoms associated with cognitive task performance across domains?
Methods
Research design
This study used a cross-sectional correlational design to examine associations between problematic Instagram use and inattentive ADHD symptom endorsement, and to explore whether these measures co-occur with performance on brief cognitive tasks. Data were collected between September and December 2024. A cross-sectional design was selected because the study was intended as a pilot to estimate effect sizes, refine measurement procedures, and generate testable hypotheses for future longitudinal and experimental work; accordingly, analyses focus on associations rather than causal inference.
Participants and recruitment
Participants were recruited via convenience sampling from a neurodiversity awareness club at Saint Paul Preparatory School (SPPS). Eligibility criteria included: (1) age 15-22 years, (2) ability to complete study tasks in English, and (3) provision of informed consent (and assent/parental consent for minors, as applicable). Thirteen participants enrolled (100% female; M = 16.5, SD = 2.1). The all-female composition reflects the characteristics of volunteers recruited from this setting during the study period rather than an a priori restriction; this limits generalizability and is addressed as a study limitation.
Variables and Measurements
Instagram Addiction Scale (IAS). Instagram-related addictive tendencies were assessed using the Instagram Addiction Scale (IAS) developed by Kircaburun and Griffiths16. The IAS consists of 15 items, with a format of a 6-point Likert scale from 1 = “never” to 6 = “always,” yielding total scores from 15 to 90. IAS scoring categories followed prior cutoffs: non-addiction (15-37), mild (38-58), moderate (59-73), and severe (≥ 74)16,17.
DSM-5 inattentive symptom checklist (modified). Inattentive ADHD symptoms were adapted for self-report administration. Item content corresponded to the nine DSM-5 inattentive criteria items1. Items were rated on a 4-point scale (0 = “Not at all,” 1 = “Just a Little,” 2 = “Often,” 3 = “Very Often”), producing a total score range of 0-27. For descriptive (non-diagnostic) classification, we counted the number of inattentive symptoms endorsed at high frequency (“Often” or “Very Often”). Because DSM symptom-count thresholds vary by age group, this endorsement rule was used as a screening-style summary rather than a DSM-based diagnosis. To operationalize inattentive symptom severity continuously, we also used the summed symptom score.
Pilot cognitive task battery. A brief, study-developed cognitive task set was used to quantify performance on timed items intended to tap attention-relevant cognitive functions. This task set was created for exploratory purposes and has not been formally validated as a diagnostic or clinical measure; it is therefore treated as a pilot cognitive screener.
The battery consisted of nine multiple-choice items administered on Quizizz, divided into three domains (three items per domain): pattern recognition, spatial reasoning, and visual recall/memorization. Domain selection was guided by prior ADHD literature linking inattentive symptoms to sustained attention and working memory/executive-function demands. Accordingly, recall items were intended to draw on short-term/working memory demands, spatial items on visuospatial manipulation and executive control, and pattern items on sustained attention/perceptual reasoning.
Each item had a fixed time limit of 30 seconds. Accuracy (correct or incorrect) and response time were recorded. Response times were automatically recorded by the Quizizz platform. Timed-out items were coded as incorrect. Quizizz logs item-level accuracy and time-to-response for each question under the fixed time limit. Because several items were adapted from third-party materials, task prompts/images are not reproduced in the manuscript. Domain structure, timing, scoring procedures, and the item set (as administered) can be shared upon reasonable request.
Scoring. For each domain, a domain score was computed as the number of correct responses (range 0-3). A total cognitive score was computed as the sum of correct responses across domains (range 0-9). Response time outcomes were summarized as the mean time in seconds across completed items overall and by domain.
Procedure
Data collection was conducted in two phases. In Phase 1, participants completed the online cognitive tasks via a Quizizz link, with a 30-second limit per item under identical timing settings (30 s per item). In Phase 2, participants completed the IAS and DSM-5 inattentive symptom checklist in a quiet classroom environment, with up to 20 minutes allotted. All participants completed the cognitive tasks before the questionnaires to reduce the possibility that completing symptom questionnaires would prime participants’ perceptions or strategies during the cognitive tasks. Task order was fixed for all participants, and counterbalancing was not used.
Data analysis
Descriptive statistics (mean, SD, range) were computed for IAS scores, inattentive symptom scores, and cognitive outcomes. Pearson correlations were used to examine associations among IAS total scores, inattentive symptom scores, and cognitive measures (two-sided α = 0.05). Because multiple correlations were tested, we treated the reported correlation tests as a single family and applied both Benjamini-Hochberg FDR and Bonferroni corrections across that set. Adjusted p-values are reported alongside unadjusted values.
Given that the cognitive total score is computed from domain scores, correlations between the total score and its component domain scores were treated as descriptive rather than independent hypothesis tests.
Ethical considerations
Ethical procedures followed relevant school research policies and standard human-subject practices. Participants aged 18 years and older provided informed consent. For participants younger than 18 years, the school-approved consent procedure was followed. Participation was voluntary, responses were de-identified before analysis, and data were stored on local devices accessible only to the research team.
Data Availability
De-identified data and analysis code are available from the author upon reasonable request.
Results
Participants
The sample included 13 female participants aged 15-22 years (M = 16.5, SD = 2.1). IAS scores ranged from 22 to 60 (M = 43.5, SD = 10.6). Based on prior IAS cutoffs, 9 participants (69.2%) fell into the mild range, 3 (23.1%) fell into the non-problematic range, and 1 (7.7%) fell into the moderate range; no participants fell into the severe range. Using the study’s screening rule on the adapted DSM-5 inattentive checklist (≥5 symptoms rated “Often” or “Very Often”), 3 participants (23.1%) met the high-endorsement criterion.
Descriptive cognitive performance
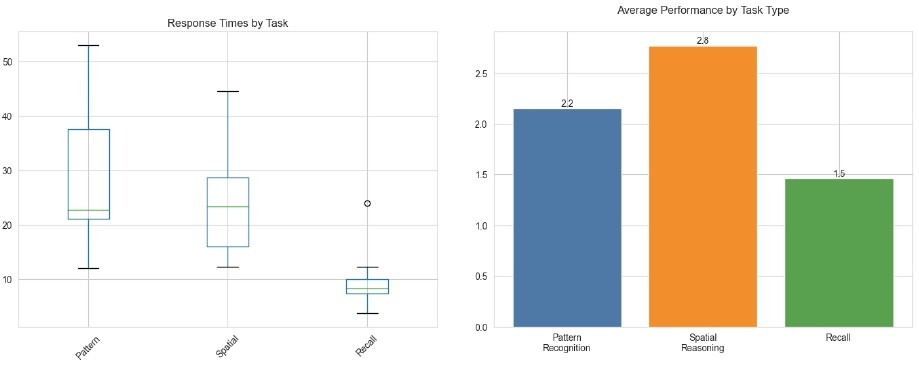
Descriptive statistics for IAS, ADHD inattentive symptoms, and cognitive task outcomes are reported in Table 1. Mean performance was highest for spatial reasoning (M = 2.77, SD = 0.83), followed by pattern recognition (M = 2.15, SD = 0.80) and recall (M = 1.46, SD = 0.78). The cognitive test total score ranged from 3 to 9 (M = 6.38, SD = 1.66). Mean response time across tasks was 21.79 seconds (SD = 8.21). By domain, pattern recognition showed the longest average response time (M = 28.57 s, SD = 13.53), and recall showed the shortest (M = 9.23 s, SD = 5.18). Figure 2 summarizes performance and response time profiles across task domains.
| Measure | Mean | Std |
| Pattern Recognition Score | 2.15 | 0.80 |
| Pattern Recognition Time (s) | 28.57 | 13.53 |
| Spatial Reasoning Score | 2.77 | 0.83 |
| Spatial Reasoning Time (s) | 25.12 | 10.20 |
| Recall Score | 1.46 | 0.78 |
| Recall Time (s) | 9.23 | 5.18 |
| Cognitive Test Total Score | 6.38 | 1.66 |
| Cognitive Test Response Time (s) | 21.79 | 8.21 |
| ADHD Total Score | 8.31 | 6.96 |
| IAS Score | 43.46 | 10.61 |
Correlational Analyses
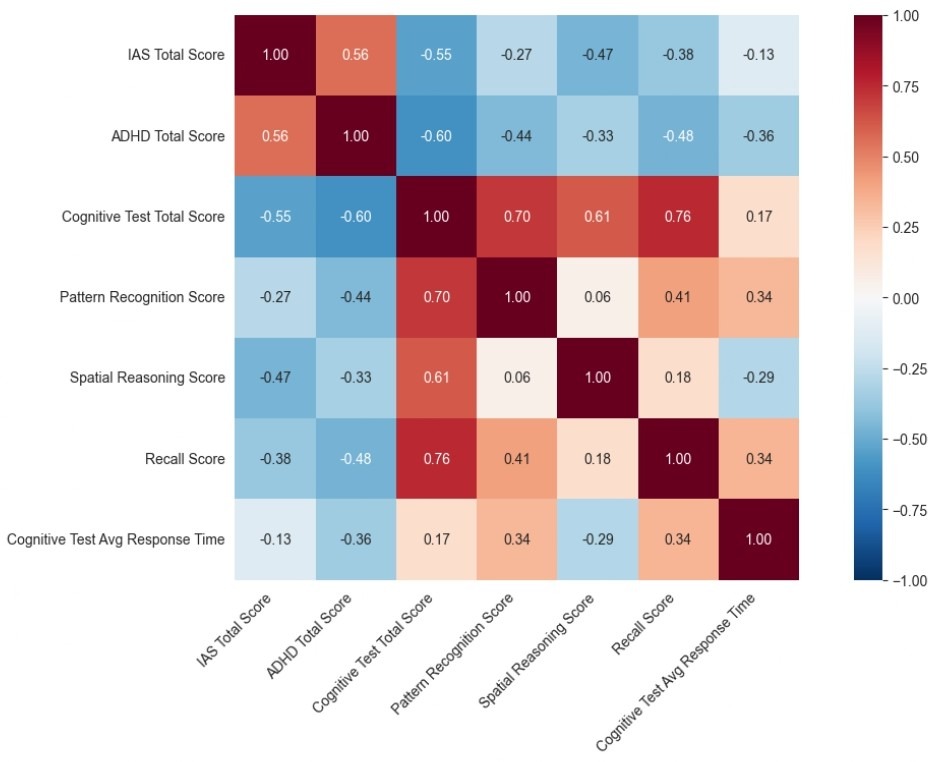
Because multiple correlations were examined, we treated all correlation tests reported in this section as a single family. We reported multiple-comparison adjustments using both the Benjamini-Hochberg false discovery rate (FDR-BH) procedure and the Bonferroni correction. Pearson correlations among key variables are visualized in Figure 3. IAS scores correlated positively with inattentive symptom scores (r = 0.561, 95% CI [0.014, 0.849], unadjusted p = 0.046; FDR q = 0.108; Bonferroni p = 0.276). ADHD inattentive symptom scores were correlated with lower overall cognitive test performance (r = -0.603, unadjusted p = 0.030; FDR q = 0.108; Bonferroni p = 0.180). IAS scores were negatively associated with cognitive test total scores (r = -0.545, 95% CI [−0.843, 0.009], unadjusted p = 0.054; FDR q = 0.108; Bonferroni p = 0.324), which did not meet α = 0.05. Correlations between IAS scores and domain-specific performance measures (pattern recognition, spatial reasoning, and recall) were negative, but none met q < 0.05 after FDR correction (Table 2A). FDR-BH and Bonferroni corrections were applied across all correlation tests reported in this section (Tables 2A-2B). Because the cognitive test total score is computed from the domain scores, correlations between the total score and its components reflect structural dependence and are reported descriptively rather than treated as independent hypothesis tests.
| Variable | r | 95% CI for r | p (two-sided) | p (FDR-BH) | p (Bonferroni) |
| Pattern Recognition Score | -0.274 | [-0.717, 0.326] | 0.365 | 0.365 | 1.000 |
| Spatial Reasoning Score | -0.468 | [-0.810, 0.112] | 0.107 | 0.161 | 0.642 |
| Recall Score | -0.382 | [-0.771, 0.214] | 0.198 | 0.238 | 1.000 |
| Cognitive Test Total Score | -0.545 | [-0.843, 0.009] | 0.054 | 0.108 | 0.324 |
| ADHD Total Score | 0.561 | [0.014, 0.849] | 0.046 | 0.108 | 0.276 |
| Variable | r | 95% CI for r | p (two-sided) | p (FDR-BH) | p (Bonferroni) |
| Cognitive Test Total Score (vs. ADHD Total Score) | -0.603 | [-0.866, -0.078] | 0.03 | 0.108 | 0.18 |
Multiple-comparison adjustment
After applying FDR-BH and Bonferroni corrections across the full family of reported correlation tests, none of the correlations met q < 0.05. Accordingly, results are interpreted in terms of effect-size estimates and uncertainty rather than adjusted statistical significance.
Discussion
This pilot study examined associations among problematic Instagram use (IAS), inattentive ADHD symptom endorsement (DSM-5 inattentive checklist), and performance on brief cognitive tasks in a small sample of female adolescents and young adults. In unadjusted analyses, we observed three directionally consistent correlations. First, higher IAS scores co-occurred with higher inattentive symptom scores. Second, higher inattentive symptom scores were associated with lower overall cognitive task performance. Third, IAS scores showed a negative association with overall cognitive performance, but this estimate was uncertain and did not survive multiple-comparison adjustment. Because the sample was small, female-only, and drawn from a single setting, these findings should be viewed as preliminary and hypothesis-generating rather than confirmatory.
Instagram addiction and inattentive ADHD symptoms
The observed IAS-inattention association is broadly consistent with prior work linking problematic or dysregulated social media use to attention-related difficulties7,8. Importantly, the present findings do not establish whether problematic Instagram use precedes changes in attention, whether pre-existing attentional vulnerabilities increase susceptibility to compulsive platform engagement, or whether both are shaped by third factors such as sleep, stress, or academic demands. A cautious interpretation is that problematic Instagram use and inattentive symptom endorsement may cluster together in some adolescents and young adults, warranting further investigation in larger and more diverse samples.
Instagram’s platform features provide plausible, testable hypotheses for why such clustering might occur. Algorithmically curated feeds and infinite scroll can encourage repeated novelty seeking and sustained engagement. Ephemeral content and frequent notifications can increase checking frequency and interrupt ongoing tasks. Short-form video loops (e.g., Reels) may promote rapid context switching and reduce opportunities for sustained attention on a single activity. Together, these features may place demands on attentional control by increasing attentional switching costs and working-memory load during multitasking, especially in individuals already prone to distractibility11,13. Meanwhile, these mechanisms remain speculative in the present study because platform features were not experimentally manipulated or objectively measured; they are offered to motivate future, more targeted designs rather than to infer causation.
A complementary possibility is a “vicious cycle” pattern: individuals experiencing everyday attention difficulties may gravitate toward highly stimulating, low-effort digital content, which can further fragment time-on-task and reinforce habitual checking behaviors. The present data are compatible with this cycle as a conceptual framework, but temporal ordering cannot be evaluated in cross-sectional data.
Cognitive performance patterns and their interpretation
Cognitive task outcomes showed two notable relationships. Inattentive symptom scores were negatively associated with overall cognitive performance, indicating that greater self-reported inattention was associated with weaker performance on brief, timed tasks. In contrast, the IAS-cognitive association was negative but did not meet α = 0.05 and did not survive multiple-comparison adjustment. This pattern should therefore be treated as uncertain and not as evidence of a reliable relationship in the population.
Domain-level results were directionally consistent. Higher IAS scores corresponded to lower scores in spatial reasoning, recall, and pattern recognition, though none of these domain-specific associations were statistically reliable in this underpowered sample. The descriptive performance profile also suggested potential differences across domains (e.g., higher spatial reasoning scores relative to recall). One possible interpretation is that these tasks draw on partially distinct cognitive processes (e.g., sustained attention/perceptual speed for pattern recognition, executive control for spatial reasoning, working memory for recall), and that individuals may show uneven performance across domains. However, given the small sample size, the exploratory nature of the analyses, and the lack of an established normed battery, it is equally plausible that the observed profile reflects task-specific difficulty, measurement noise, or speed-accuracy tradeoffs rather than stable cognitive differences. These considerations underscore that the cognitive outcomes in this study should be interpreted as preliminary indicators that guide refinement of measurement rather than as definitive markers of ADHD-related cognition.
Strength of evidence and the role of multiple comparisons
To reduce interpretive risk in a setting with multiple correlations and a small sample size, we applied multiple-comparison procedures (FDR-BH and Bonferroni) to the family-centered correlation set. Under these adjustments, none of the correlations reported in the Results section met q < 0.05. Accordingly, the most appropriate way to read the present results is through estimated effect sizes and their uncertainty rather than dichotomous “significant/non-significant” claims. This framing aligns with the study’s purpose as an initial exploration intended to inform future confirmatory work with adequate power.
Alternative explanations and potential confound
Several alternative explanations could account for the observed associations. First, sleep disruption is a plausible common cause: problematic social media use can be linked to later bedtimes and poorer sleep quality9,10. Sleep disruption is also associated with attention difficulties and poorer cognitive performance18,19. Second, mood symptoms (e.g., anxiety or depression), stress, and academic pressures could influence both social media engagement patterns and self-reported inattention, potentially inflating observed associations. Third, individual differences in baseline cognitive ability, motivation, or test-taking familiarity may have affected task performance independent of ADHD-related cognition. Fourth, the study did not distinguish passive scrolling from active engagement, nor did it measure frequency, timing, or context of use—factors that may differentially relate to attention and cognition.
Limitations
This study has several limitations that constrain interpretation. The sample size (N = 13) limits statistical power and increases uncertainty around effect-size estimates, raising the risk of spurious findings and unstable correlations. The sample was exclusively female and recruited from a single setting, limiting external validity and generalizability to other genders, age groups, and recruitment contexts. Measures of Instagram use and ADHD symptoms relied on self-report, which may be influenced by recall bias or social desirability. In addition, the fixed task order may have introduced fatigue or order effects, which should be addressed in future work through counterbalancing. Finally, the cognitive tasks were designed for this study and are not a validated cognitive battery; without established reliability, validity, and normative benchmarks, task scores should be interpreted cautiously as a pilot cognitive screener rather than as definitive evidence of ADHD-related cognitive deficits. These limitations collectively emphasize that the present findings are preliminary.
Future directions
The current results motivate several concrete next steps. First, replication in larger, more diverse samples is essential, with recruitment spanning genders, socioeconomic backgrounds, and varied contexts. Second, longitudinal designs should examine temporal ordering by measuring Instagram use, sleep, mood, and attention symptoms repeatedly over time. Third, experimental or intervention studies could directly test mechanisms by manipulating exposure to specific platform features (e.g., disabling notifications, limiting short-form video access, or introducing usage caps) and assessing changes in sustained attention and working memory tasks before and after the manipulation. Fourth, future work should incorporate validated cognitive batteries with known sensitivity to ADHD-related cognitive profiles and include counterbalancing to control order effects. Finally, distinguishing patterns of Instagram engagement (passive vs. active use; daytime vs. late-night use; short sessions vs. prolonged sessions) may clarify which aspects of use are most closely linked to attentional difficulties.
Implications
Within the constraints of a small, cross-sectional pilot sample, the present study offers preliminary indications that problematic Instagram use and inattentive symptom endorsement may co-occur and that inattentive symptoms may align with lower performance on brief cognitive tasks. These results should not be used to infer causality or to draw clinical conclusions. Instead, they can inform hypothesis refinement, measurement improvements, and the design of larger confirmatory studies that test whether specific patterns or features of Instagram engagement relate to attention and cognition.
Conclusions
This pilot cross-sectional study examined whether problematic Instagram use is associated with inattentive ADHD symptom endorsement and with performance on brief timed cognitive tasks among female adolescents and young adults. Overall, higher IAS scores were associated with higher inattentive symptom scores, and higher inattentive symptom scores were associated with lower cognitive task performance. The pattern between problematic Instagram use and cognitive performance was directionally negative, but did not survive multiple-comparison adjustment, underscoring the exploratory nature of the findings.
These results should be interpreted cautiously. The small convenience sample, female-only recruitment context, reliance on self-report symptom measures, cross-sectional design, and use of a study-developed (non-validated) cognitive task battery limit generalizability and prevent causal or directional conclusions. Accordingly, the present estimates are best viewed as preliminary effect-size information to guide more rigorous follow-up research.
Future studies should replicate these associations in larger and more diverse samples and use longitudinal and/or experimental designs to clarify temporal ordering. Incorporating objective measures of platform use (e.g., usage logs), validated cognitive batteries, and counterbalanced task administration would strengthen measurement and reduce potential confounds. If replicated, this line of work may help inform interventions that support healthier social media engagement and attention-related outcomes in adolescents and young adults.
Acknowledgments
We would like to express our sincere gratitude to the administrators and faculty at Saint Paul Preparatory School for facilitating access to participants and providing a supportive environment for this research. Special thanks go to the members of the Neurodiversity Awareness Club, whose willingness to participate and share their experiences made this study possible.
References
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. American Psychiatric Association Publishing, 2022. https://doi.org/10.1176/appi.books.9780890425787. [↩] [↩]
- A. Niina, O. Eyre, R. Wootton, E. Stergiakouli, A. Thapar, L. Riglin. Exploring adhd symptoms and associated impairment across development. Journal of Attention Disorders. Vol. 26, pg. 822–830, 2022, https://doi.org/10.1177/10870547211025612. [↩]
- P. O. Quinn, M. Madhoo. A review of attention-deficit/hyperactivity disorder in women and girls: uncovering this hidden diagnosis. The Primary Care Companion For CNS Disorders. 2014, https://doi.org/10.4088/PCC.13r01596. [↩]
- S. Young, N. Adamo, B. B. Ásgeirsdóttir, P. Branney, M. Beckett, W. Colley, S. Cubbin, Q. Deeley, E. Farrag, G. Gudjonsson, P. Hill, J. Hollingdale, O. Kilic, T. Lloyd, P. Mason, E. Paliokosta, S. Perecherla, J. Sedgwick, C. Skirrow, K. Tierney, K. Van Rensburg, E. Woodhouse. Females with adhd: an expert consensus statement taking a lifespan approach providing guidance for the identification and treatment of attention-deficit/ hyperactivity disorder in girls and women. BMC Psychiatry. Vol. 20, pg. 404, 2020, https://doi.org/10.1186/s12888-020-02707-9. [↩]
- D. Kuss, M. Griffiths. Social networking sites and addiction: ten lessons learned. International Journal of Environmental Research and Public Health. Vol. 14, pg. 311, 2017, https://doi.org/10.3390/ijerph14030311. [↩]
- T. J. Dekkers, J. Van Hoorn. Understanding problematic social media use in adolescents with attention-deficit/hyperactivity disorder (adhd): a narrative review and clinical recommendations. Brain Sciences. Vol. 12, pg. 1625, 2022, https://doi.org/10.3390/brainsci12121625. [↩] [↩]
- C. K. Ra, J. Cho, M. D. Stone, J. De La Cerda, N. I. Goldenson, E. Moroney, I. Tung, S. S. Lee, A. M. Leventhal. Association of digital media use with subsequent symptoms of attention-deficit/hyperactivity disorder among adolescents. JAMA. Vol. 320, pg. 255–263, 2018, https://doi.org/10.1001/jama.2018.8931. [↩] [↩]
- M. Boer, G. Stevens, C. Finkenauer, R. Van Den Eijnden. Attention deficit hyperactivity disorder‐symptoms, social media use intensity, and social media use problems in adolescents: investigating directionality. Child Development. Vol. 91, pg. e853–e865, 2020, https://doi.org/10.1111/cdev.13334. [↩] [↩]
- O. Ahmed, A. Dawel, E. I. Walsh, N. Cherbuin. Longitudinal associations between problematic social media use and mental health: mediating role of sleep. Addictive Behaviors. Vol. 170, pg. 108446, 2025, https://doi.org/10.1016/j.addbeh.2025.108446. [↩] [↩]
- L. Raudsepp. Brief report: problematic social media use and sleep disturbances are longitudinally associated with depressive symptoms in adolescents. Journal of Adolescence. Vol. 76, pg. 197–201, 2019, https://doi.org/10.1016/j.adolescence.2019.09.005. [↩] [↩]
- M. T. Maza, K. A. Fox, S.-J. Kwon, J. E. Flannery, K. A. Lindquist, M. J. Prinstein, E. H. Telzer. Association of habitual checking behaviors on social media with longitudinal functional brain development. JAMA Pediatrics. Vol. 177, pg. 160–167, 2023, https://doi.org/10.1001/jamapediatrics.2022.4924. [↩] [↩]
- Md. K. Hasan. Digital multitasking and hyperactivity: unveiling the hidden costs to brain health. Annals of Medicine & Surgery. Vol. 86, pg. 6371–6373, 2024, https://doi.org/10.1097/MS9.0000000000002576. [↩]
- B. C. W. Ralph, D. R. Thomson, J. A. Cheyne, D. Smilek. Media multitasking and failures of attention in everyday life. Psychological Research. Vol. 78, pg. 661–669, 2014, https://doi.org/10.1007/s00426-013-0523-7. [↩] [↩]
- M. Barneron, N. Saka, S. Shlepack, A. Khattab, Y. Pollak. Increased intra-individual variability among individuals with adhd: first evidence from numerosity judgment and verbal and quantitative reasoning. Psychological Medicine. Vol. 54, pg. 3689–3696, 2024, https://doi.org/10.1017/S0033291724001892. [↩]
- Drew. W. R. Halliday, Y. Kim, S. W. S. MacDonald, M. A. Garcia-Barrera, S. R. Hundza, S. J. Macoun. Intraindividual variability in executive and motor control tasks in children with attention deficit hyperactivity disorder. Journal of Clinical and Experimental Neuropsychology. Vol. 43, pg. 568–578, 2021, https://doi.org/10.1080/13803395.2021.1965097. [↩]
- K. Kircaburun, M. D. Griffiths. Instagram addiction and the big five of personality: the mediating role of self-liking. Journal of Behavioral Addictions. Vol. 7, pg. 158–170, 2018, https://doi.org/10.1556/2006.7.2018.15. [↩] [↩]
- M. Zarenti, F. Bacopoulou, M. Michou, I. Kokka, D. Vlachakis, G. P. Chrousos, C. Darviri. Validation of the instagram addiction scale in greek youth. EMBnet.Journal. Vol. 26, pg. e973, 2021, https://doi.org/10.14806/ej.26.1.973. [↩]
- J. Lim, D. F. Dinges. A meta-analysis of the impact of short-term sleep deprivation on cognitive variables. Psychological Bulletin. Vol. 136, pg. 375–389, 2010, https://doi.org/10.1037/a0018883. [↩]
- J. Roca, L. J. Fuentes, A. Marotta, M.-F. López-Ramón, C. Castro, J. Lupiáñez, D. Martella. The effects of sleep deprivation on the attentional functions and vigilance. Acta Psychologica. Vol. 140, pg. 164–176, 2012, https://doi.org/10.1016/j.actpsy.2012.03.007. [↩]