Authors: Sejal Ahluwalia and Shrestha Vatsala
Peer Reviewer: Anmol Guard
Professional Reviewer: Kevin Malone
Abstract:
Current cardiovascular sutures are greatly incompatible with heart tissue sensitivities. Of 700,000 cardiovascular surgeries conducted annually, 41,000 result in infection after coronary bypass. Steel and plastics are widely used, suggesting no recent advancements in this technology. In last year’s award-winning project, keratin (a wound-healing protein) was tested on muscle tissue. Results showed that keratin caused the cells to proliferate, suggesting improved wound repair. This year, keratin-infused fibers were electrospun. A solution of 10% (by weight) polycaprolactone (PCL) in glacial acetic acid (GAA) was created along with a solution of 10% keratin powder in GAA. Solutions were combined in varying ratios (80:20, 70:30, 60:40) to test for effects on nanofiber structure and tensile strength. The preliminary testing of the fibers shows that the 80:20 concentration had a tensile strength of 3.06MPa, and the 70:30 concentration had a tensile strength of 1.32MPa, both spun onto a copper plate. The 60:40 concentration fiber had a tensile strength of 0.32MPa. Since 70:30 had a higher tensile strength, more evenly spread fibers from SEM imaging, and higher keratin content, it was the ratio used for further testing. The solution was spun onto a makeshift rotating drum, and the fiber was tested yielding a tensile strength of 1.90MPa. Once the optimized suture was spun, a degradation analysis was conducted using phosphate buffered saline (PBS), and qualitative results showed evidence of the sutures being used as absorbable sutures.
Introduction:
Annually, approximately 500,000 open heart surgeries are performed in the United States, including over 200,000 coronary bypass surgeries (Chu, 2018). These procedures require the use of cardiac sutures, causing them to be considered risky endeavors. In 1896, Ludwig Rehn, a German surgeon, conducted the first successful suturing of a stab wound of a man’s heart, paving the way to modern cardiovascular surgery (Ravishankar, 2014).
Surprisingly, suture materials have not drastically changed since the 1970s (Rubin, 2016). Acknowledging this, a small study between 2007 and 2009 observed how many patients were adversely affected by infected sutures; it was found that 5.88% of 357 cardiac patients were infected by their cardiac sutures during bypass surgeries (Assunção, 2011). As the number of cardiac surgeries increases over time, more adults are being impacted by cardiac suture infections annually. 5.88% may seem acceptably low, but it corresponds with nearly 41,000 people infected. Clearly, this field of study is in need of advancement and thus, keratin sutures could potentially revolutionize cardiovascular surgeries.
Background Research:
Sutures:
The term “suture” delineates any strand of material – synthetic, silk, steel wire, etc. – used to tie blood vessels or bring tissues close together. Sutures and ligatures are specifically used to close wounds post-surgery and let them heal. Sutures require certain optimal qualities, including a high tensile strength in vivo, uniform diameter, high sterility, high pliability, freedom from impurities, and predictable performance. It is crucial that sutures and ligatures be pliable for ease of handling and knot security, since sutures are knotted into both sides of the wound (Ethicon, 2005). It is critical for sutures to be free of impurities because they can easily be rejected by the immune system. Additionally, they must not contain any irritating substances in order to promote tissue acceptance.
There are two types of sutures: absorbable and nonabsorbable. Absorbable sutures are used to hold wounds together temporarily. After the wound has closed and is able to withstand the stresses of normal use, the sutures either biodegrade, or are absorbed into the tissue; this requires the timing of absorption of the suture material to match the expected recovery time. Existing absorbable sutures include those prepared from the collagen of healthy mammals (ex. sheep intestine) or from synthetic polymers (ex. VICRYL suture made from a copolymer consisting of and coated with glycolide and lactide). Nonabsorbable sutures are those not digested by body enzymes or hydrolyzed by tissue. These nonbiodegradable materials are ultimately surrounded and enclosed by tissue fibroblasts. One of two outcomes of nonabsorbable sutures occur – removal after sufficient healing or permanent encapsulation in the tissue. Current nonabsorbable sutures are made from metal (ex. stainless steel wire), synthetic materials (ex. Nylon), or organic fibers (ex. raw silk) formed into strands by spinning, twisting, or braiding (Ethicon, 2005).
Keratin:
As a fibrous, flexible, and strong protein that forms the main structural component of hair, feathers, etc., keratin could potentially become a highly-effective cardiac suture material. Keratin is also the material that protects epithelial cells, the cells on the outer layer of a body’s surface. This biomaterial comes in various morphologies, including gels, films, coatings, aqueous forms, and, most importantly, fibers (Hill, 2010). This organic polymer has been investigated for limited potential medical applications, such as wound healing, tissue regeneration, tissue engineering, hemostasis, peripheral nerve repair, and controlled drug release (Shavandi, 2017). In these articles, it has been stated that keratin has generally good compatibility with cells and tissues, but not much research has been conducted on its potential application as a suture material (Hill, 2010). Additionally, keratin is readily available, as it can be obtained via a plethora of methods. Extraction methods include the use of controlled enzymatic hydrolysis of wool, where liquid keratin is the product. This experiment involved the use of aqueous keratin to simply test the effects of keratin on muscular tissue.
Cardiac Myocytes & Mouse Myoblasts:
Cardiac muscles are a type of special striated muscle that perform all coronary-related responsibilities. Cardiac myocytes are one of the most physically energetic cells in the body due to their assigned task of contracting the whole cardiac muscle. These myocytes make up the majority of heart tissue. They portray contractile, electrophysiological, and morphological properties, such as being able to pump blood on their own and produce electrical activity that can be detected and used to revive a heart (Mitcheson, 1998). The most similar type of cell available is mouse muscular tissue. Skeletal muscle cells and cardiac muscle cells are both striated due to a similar arrangement of contractile proteins (Starkebaum, 2017). Striated muscle tissue is comprised of transverse dark and light bands, as well as elongated with multinucleated fibers (Mitcheson, 1998). The two types of cells differ in that skeletal cells are controlled by voluntary movement whereas cardiac cells produce involuntary movement; this property, however, is not being tested and does not play a role on a cellular level in this examination. A difference between the two types of muscle which may make the results inconclusive for cardiac muscle is that cardiac cells do not heal as fast as skeletal muscle cells. Since the degree to which the cells accept the keratin is being measured, the results may vary for the two types of cells, but the extensive similarity between the two may allow for accurate conclusions.
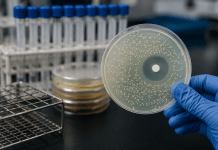
Electrospinning:
Electrospinning is a fiber production method which utilizes electric charge to draw a solution into threads onto a surface. The setup of the electrospinner with the copper plate is shown in Figure 1, while the setup of the electrospinner with the rotating drum is shown in Figure 2. A syringe pump was placed 23 cm from the surface onto which the polymer solution was spun (rotating drum or copper plate). The syringe pump contained 8 mL of polymer solution and the syringe flow rate, syringe diameter, and length were set according to syringe measurements (Thompson, 2016). A voltage was applied at both the tip of the syringe needle as well as on the opposing surface. This way, both ends of the system were charged so the solution would be drawn to the opposing surface in threads as the syringe pump ejected it.

Copper Plate & Makeshift Rotating Drum:
Electrospinning on a copper plate is quite different from electrospinning onto a rotating drum. When using a copper plate, there is far more beading, greater chance of spraying, and fewer evenly distributed fibers in the resulting polymer. A rotating drum, however, spins vertically as the thread is drawn to it, allowing for less beading, reduced chance of spraying, and more evenly distributed individual fibers in the result. Therefore, a rotating drum was created in this study to further enhance the nanofiber.
The makeshift rotating drum consisted of a 50-cm axle, a 10-cm aluminum tube, a 15-cm 3D-printed surrounding support, bearings, and 2 1.25-cm 3D-printed holders for the axle. The open part of the axle was inserted into a drill so the aluminum tube would spin at the speed setting at which the drill was set.

To apply voltage to a copper plate, alligator clips, connected to a voltage box, were clipped to the back side of the plate. To apply voltage to the rotating drum, a brush contact system was fashioned from readily available materials including metal paper clips.
Additionally, prior to spinning onto either surface, both the rotating drum and copper plate were wrapped in aluminum foil to ensure that the polymer could be reliably removed for testing.
Experimental Design:
This experiment consisted of two phases: testing the effect of aqueous keratin on Mus musculus cells, and electrospinning and mechanically testing a keratin nanofiber for use as a suture. The long-term goal of this experiment is to suggest keratin as a suitable suture material and ultimately indicate a decrease in the risk of infection.
Part One:

Part Two:

Experimental Design Part One:
The independent variable of the experiment was the concentration of aqueous keratin introduced to the cells. The dependent variable that was quantitatively measured was the viability of the cells through the use of absorbance markers, specifically the Vybrant MTT Cell Viability Assay. The control of this experiment was a flask of untreated mouse myoblasts allowed to grow as normal. A comparison was made between the noted values of the untouched mouse myoblasts and the numbers produced by those that were introduced to varying amounts of aqueous keratin. Some of the constants that recurred in this experiment were the type of mouse myoblasts, the growth medium for the cells, the incubators in which the cells were stored in, the types of culture flasks that were used, the pipettes, and the fume hood. These all stayed constant to decrease the chance of seeing the effects of more than a single variable in the experiment. They also gave a more accurate comparison of the two different cell growths. If the aqueous keratin does not substantially decrease the viability of the cells, then keratin can be an ideal solution for sutures needed in cardiovascular surgery.
Experimental Design Part Two:
The independent variable of the second phase of this experiment was the concentration of keratin powder in the solution of GAA (glacial acetic acid) and PCL (polycaprolactone) prior to it being electrospun into a fiber. Once the optimal concentration was found in quantitative and qualitative results, the surface onto which the solutions were spun changed from a copper plate to a rotating drum to promote even distribution of the threads. To further enhance the suture, two other independent variables were tested: the settings of syringe flow rate and rotational velocity of the drum. To test the nanofibers, SEM, tensile strength, and degradation analyses were conducted. When SEM images were taken of the nanofibers to determine which were optimal, the distribution, amount of beading, and the thickness of the individual fibers were the dependent variables. A tensile tester was used to find the tensile strength of the fibers (in MPa), the dependent variable in this test. Lastly, in the degradation analysis, the dependent variable was the quality shown in the SEM images taken, based on distribution of the threads, the amount of beading, and the thickness of the fibers. The overarching control throughout this study was the tensile strength of current cardiovascular sutures, specifically the silk suture. Constants in this experiment were the type of the PCL, the type of keratin powder, and time the fibers spent in degradation analysis.
Methodology
Methodology Part One:
The procedures were conducted under a sterilized fume hood. The cells were prepared and warmed after being taken out of cryopreservation, put into culture flasks, and stored in an incubator. A cell culture growth medium was made to feed them every two to three days. Each time the cells reached 80% confluency, they were subcultured into two other flasks in a 1:6 ratio. Consequently, once the cells had reached optimum growth, the cells were harvested into a well plate, with each well receiving 10 uL of cell solution. Keratin was introduced to 24 different wells (each set of 8 introduced to a different concentrated solution) with each well receiving 90 uL of solution. The control of the experiment was a separate set of 8 wells of cells treated with 90 uL regular growth medium. To gather and analyze the data of how the cells responded to the keratin, an absorbance marker was implemented. The MTT Cell Viability Assay was added to determine the amount of absorption by the cells – more absorption means more cells in vitro, which suggests that keratin could be a potential suture material.
Methodology Part Two:
The copper plate and makeshift rotating drum were incorporated into the electrospinner interchangeably to see their different effects on fiber composure. A tensile tester was used to test the tensile strength of each nanofiber spun. The values were divided by the cross sectional area of the fiber tested to calculate its tensile strength, in MegaPascals. The samples were then cut into small squares, gold-coated with the sputter coater, and analyzed in the Scanning Electron Microscope (SEM). The SEM creates images on the micrometer scale to depict the composure of small samples. Phosphate Buffered Saline (PBS) was used for the degradation analysis because it was isotonic to body fluids present in the human body.
Procedures
Procedures Part One:
Creating the Growth Medium
- The researchers were equipped with all appropriate PPE and prepared the fume hood.
- All equipment was sterilized before entering the fume hood.
- A 25 mL pipette was used to pipette 90 mL of DMEM into a media bottle.
- A 10 mL pipette was used to aspirate 10 mL of FBS into the same media bottle.
- The solution was mixed thoroughly creating 100 mL of growth medium.
- 2 mL of the solution was put into a media test vial and incubated to ensure it was not infected.
- All equipment was extracted and the fume hood was sterilized with ethanol.
Handling Procedure for Frozen Cells
- To ensure the highest level of viability, the vial was thawed and initiated as soon as possible upon receipt. It was not stored at 70°C because it could have resulted in loss of viability.
- The vial was thawed in a 37°C water bath for 2 minutes. To reduce the possibility of contamination, the cap was kept out of the water.
- The vial was removed from the water bath as soon as the contents were thawed and was decontaminated by dipping in or spraying with 70% ethanol.
- The vial contents were transferred to a centrifuge tube containing 9.0 mL of the culture medium and spun at approximately 125•g for 6 minutes.
- The supernatant, or extra fluid, was discarded and the cell pellet was pipetted into a new culture flask with 6 mL of fresh growth medium.
- The cell suspension was transferred to an appropriate size vessel. The culture vessel containing the growth medium was placed into the incubator for at least 15 minutes to allow the medium to reach its normal pH (7.0 to 7.6).
- The culture was incubated at 37°C in a suitable incubator (5% CO2) for 2-3 days.
Feeding the Cells
- The cell culture media was taken out of the fridge and placed in the 37°C water bath to allow it to reach optimal temperature.
- The cells were then removed from the incubator and prepared for experimentation under the fume hood.
- The contamination, turbidity, and morphology of media and cells were observed.
- If the cells had reached 80% confluency or more, the subculturing procedure was executed/implemented. Otherwise, the hood was sterilized with 70% ethanol.
- The media was removed from the hot water bath and sterilized with 70% ethanol.
- The culture flask was tilted back and the media was aspirated from the flask using a 10 mL pipette. It was then properly discarded.
- 6 mL of prewarmed media were added to the culture flask in a way that it encompassed the whole bottom surface.
- The cells were observed under the microscope to confirm health with gentle handling and then placed back into the incubator.
Subculturing Procedure
- The culture medium at the bottom of the culture flasks was pipetted out and discarded.
- The layer of cells was briefly rinsed with 0.25% (w/v) Trypsin (0.53 mM EDTA) solution to remove all traces of serum which contained trypsin inhibitor and to detach the cells from the flask.
- 2.0 to 3.0 mL of Trypsin-EDTA solution were added to the flask. The cells were observed under an inverted microscope until the cell layer dispersed (usually within 5 to 15 minutes).
- 6.0 to 8.0 mL of complete growth medium were added to the cells and aspirated by gentle pipetting.
- A ratio of 1: 6 was used to distribute the suspended cells into two new culture vessels.
- To avoid clumping, the cells were not agitated (hit or shook) while waiting for the cells to detach. Cells that were difficult to detach were placed in an incubator at 37°C to facilitate dispersal.
- This medium removal process occurred every two to three days.
Creating Aqueous Keratin Solutions
- A stock solution was created adding 0.05 mL DMSO, 0.07 mL aqueous keratin, and 49.88 mL of growth medium into a media bottle A. This created a 78 uM keratin concentration.
- From media bottle solution A, 14.7 mL were extracted and put into media bottle B using a 1:3 ratio.
- 29.3 mL of normal media was aspirated into media bottle B, thus creating a keratin concentration of 26 uM.
- 14.7 mL of solution B was pipetted into an empty media bottle C.
- 29.3 mL of normal growth medium was added to media bottle C creating a 8.7 uM keratin solution.
Harvesting the Cells
- Place all necessary equipment into fume hood including micropipettes, four media solution bottles, a confluent culture flask, etc.
- The growth medium was removed from the culture flask and 2 mL of trypsin was added.
- The flask was tilted back and forth to encourage detachment of cells.
- Trypsin was removed and 2 additional milliliters of trypsin were added to the flask.
- The flask was incubated until all cells were detached.
- Afterwards, 8 mL of growth medium were added to neutralize the trypsin.
- 5 mL of cells were placed into a reagent tray.
- The 8-tip P100 micropipette was used to take 10 uL of the cells and put into 32 wells in the 96 well plate (8000 cells per well).
- A P200 single-tip micropipette was used to put 90 uL of each solution into their corresponding wells.
- The well plate was incubated for 48 hours.
Applying Vybrant MTT Cell Viability Assay
- A 12 mM MTT stock solution was prepared by adding 1 mL of sterile PBS to one 5 mg vial of MTT included in the kit. The PBS and MTT were mixed together.
- 10 mL of 0.01 M HCl was added to 1 tube containing 1 gm of SDS included in the kit. The solution was mixed.
- The medium was removed from each well and replaced with 90 uL of corresponding media.
- 10 uL of the 12 mM MTT stock solution was added to each well.
- The well plate was incubated at 37°C for 4 hours.
- 100 uL of the SDS-HCl solution was added to each well and mixed thoroughly using the pipette.
- The well plate was incubated for 3 hours.
- Each sample was mixed again using a pipette and absorbance was read at 570 nm.
Reading the Well Plate Using Microplate Reader
- The online application for the Synergy HT Microplate Reader was set up according to protocol.
- The wavelength for absorbance detection was set at 570 nm according to the protocol for the Microplate Reader was used in the study.
- The created protocol was run and data was collected in an Excel spreadsheet regarding Mean OD (optical density), CV (coefficient of variation) OD, and %CV OD.
Procedures Part Two:
Preparation of Keratin Solutions
- Keratin was weighed and the weight was recorded.
- Glacial acetic acid was added to the keratin powder to create a 10% by weight keratin solution.
Preparation of 10% wt PCL Solution
- PCL (<#EPSILON>-caprolactone polymer, Mn 70 – 90 kDa), and glacial acetic acid were obtained.
- A 10% by weight PCL in glacial acetic acid solution was made by stirring overnight and a homogeneous mixture was created.
Preparation of Keratin/PCL Solution
- The 10% by weight PCL solution and 10% by weight keratin solution were obtained. The keratin was added into the PCL solution drop wise in order to create 10 ml PCL/keratin solutions of 80:20, 70:30, and 60:40 ratios.
- A vortexer was used to obtain a homogeneous mixture of PCL/Keratin solution before electrospinning.
Production of Electrospun PCL/Keratin Fiber On a Copper Plate
- 8 mL of the PCL/keratin solution was placed in a 10 mL disposable syringe fitted with a 0.5-mm diameter plastic tube. The syringe was placed in a syringe pump where the flow rate was set to constant 2.5 mL/hr.
- 19 – 22 kV voltage was applied across the tip of the needle and the back of the copper plate.
- The copper plate was wrapped with aluminum foil before the solution was spun. Labeling tape was used to secure the aluminum foil.
Production of Electrospun PCL/Keratin Fiber On a Rotating Drum
- 8 mL of the PCL/keratin solution was placed in a 10 mL disposable syringe fitted with a 0.5-mm diameter plastic tube. The syringe was placed in a syringe pump where the flow rate will be set to 2.5 mL/hr for one trial and 2 mL/hr for another trial.
- Voltage was applied to the tip of the needle connected to the syringe (positioned ~23 cm from the fiber collecting drum, and ~30 degree from the horizontal). A 19 – 22 kV voltage was applied to the syringe needle and the collector drum. The drum was rotated at around 200 rpm for the 2.5 mL/hr flow rate, and 1500 rpm for the 2 mL/hr flow rate to test various settings.
- The collector drum was wrapped with aluminum foil before the sample was run. To ensure that the aluminum foil was stable, the labeling tape was applied on either end.
Mechanical Analysis of PCL/Keratin Nanofibers
- The sample was cut into 3 cm by 3 cm. A digital micrometer was used to record the thickness. For each composition prepared, five samples were used.
- The 3 x 3 cm sample was attached to the tensile tester. A custom designed specimen holder was used to attach the sample. The sample was sandwiched between specimen holders. The 10 N load cell with a displacement rate of 10 mm/min was applied.
- The extension and load values were recorded through software according to software protocol.
Surface Morphology and Structural Characterization
- A scanning electron microscope (SEM) with parameters of accelerating voltage of 15 kV and current of 5 µA to observe the morphology of the electrospun fibers was used.
- Prior to imaging with SEM, a 2 cm2 section of the fiber was cut and attached to a SEM stage using copper tape. The stage was placed inside the sputter coater and was coated with gold at 15 mA for 1 min and 30 sec to create a gold layer approximately 11 nm thick utilizing the protocols specific to the sputter coater used. The sample was loaded into the chamber of the SEM.
- An image was taken and saved to a computer.
Degradation Analysis of Nanofibers
- Dried PCL/keratin nanofiber membranes were cut into squares approximately 3 cm x 3 cm.
- The 9 cm2 samples were sterilized with 80% alcohol for a 10 min incubation period and were washed thoroughly with DI water. The samples were incubated in 15 ml of PBS, pH 7.5, at 35 ºC in an incubator and at room temperature.
- The membranes were taken out of the solution after 7 days.
- The samples were dried and attached to a SEM stage using copper tape. The stage was placed inside the sputter coater and was coated with gold at 15 mA for 1 min and 30 sec according to the sputter coater protocols.
- The sample was loaded into the chamber of the SEM. The fiber samples were observed at an accelerating voltage of 1.5 kV and 5 µA current.
Results
This experiment was two-fold, spanning over two years, with the first facet centered around aqueous keratin tested on C2C12 mouse muscle cells (Mus musculus), and the other based around testing a spun keratin nanofiber. The former was aimed to be used as a premise for determining whether aqueous keratin negatively affected cells, whereas the latter served the purpose of understanding and engineering the optimal keratin-based suture.
Results: Part One
This experiment tested the effect of varying concentrations of aqueous keratin (C3H7NO2S) on C2C12 mouse muscle cells. The independent variable was the different aqueous keratin concentrations and the dependent variable was the cell viability.
The trials were conducted in a 96 well plate, of which only 32 wells were used (8 for each concentration of aqueous keratin). The microplate reader reported the results below. Table 1 shows the absorbance of the assays by the cells, and this was read through the measurement of optical density at a wavelength of 570 nm. Darker blue hues represent more absorbance in those wells, which reflect a relatively higher cell viability.
Each row of each graph below represents a different concentration of aqueous keratin. Row F depicts the cells introduced to the control solution. Row E portrays the cells introduced to treatment A (78 uM aqueous keratin). Row D shows the cells introduced to treatment B (26 uM aqueous keratin). Row C delineates the cells introduced to treatment C (8.7 uM aqueous keratin).
In Tables 1, 2, 3, and 4, OD is an abbreviation for optical density, the measurement unit used by the microplate reader. In Tables 3 and 4, CV represents the coefficient of variability. The percentage used in Table 3 is the CV divided by 100. Having a %CV that is below 1% is the preferred outcome between replicated samples and is one measure to demonstrate that the assay was well-run and the results are precise and accurate.


Results: Part Two
The following nanofibers, shown in Images 1, 2, and 3, were spun onto a copper plate whereas those shown in Images 4 and 5 were spun on the makeshift rotating drum. Mechanical and degradation analyses were conducted.
To further enhance the suture, the 70:30 concentration nanofiber was spun onto a makeshift rotating drum. The syringe flow rate (mL/hr) and rotational velocity (rpm) were adjusted on the rotating drum to see which would better the distribution of the threads in the fibers.



Table 5. The tensile strengths of the 70:30 fiber electrospun at two different RPMs and two different flow rates

A degradation analysis was performed on the fiber shown in Image 5, where a section was put into PBS and kept at room temperature (25°C) and another was put into PBS and kept in an incubator at 35°C. The before and after SEM images were compared.

Discussion
Discussion: Part One
In this investigation, the effect of varying concentrations of aqueous keratin (C3H7NO2S) on C2C12 mouse muscle cells (Mus musculus) was observed. The independent variable was the different aqueous keratin concentrations and the dependent variable was the cell viability.
According to Table 1, the absorbance of treatments A, B, and C were all relatively similar to the control group. The average absorbance for the control was 1.235 OD. The average absorbance for treatment A, the most concentrated solution (78 uM), was 1.350 OD. The percent difference in cell viability between the control and solution A datasets differed by 9.311%. The average absorbance for treatment B, 26 uM aqueous keratin, was 1.300 OD. The percent difference in cell viability between the control and solution B datasets increased by 5.263%. The average absorbance for treatment C, 8.7 uM aqueous keratin, was 1.216 OD. The percent difference in cell viability between the control and solution C datasets decreased by 1.538%. In Table 1, row E, there was an outlier in column 10 which had an absorbance of 0.776 OD which was likely caused due to errors explored below.
According to Table 2, the mean OD’s for the second dataset, the average cell viability for the cells treated with solution A, the most concentrated, was 1.264 OD. The average cell viability treated with solution B was 1.026 OD. The average cell viability for cells treated with solution C was 0.986 OD. The control had an average cell viability, with all 8 wells, of 0.928. The percent difference between the control and cells treated with solution A was a significant 36.211% increase. The percent difference in cell viability between the cells treated with solution B and the control was a 10.521% increase. Lastly, the percent difference in viability between the cells treated with solution C and the control was a 6.291% increase.
Tables 3 and 4 work together to represent more accurate and precise data since the %CV for each dataset is comparatively low. This means that there is more precision and accuracy among the replicated samples (omitting the outlier previously stated).
Sources of error that may have occurred in this investigation include sterility, time frame, failure to calibrate instrument, and personal error. Inconsistent sterility can come from not thoroughly sterilizing all equipment brought into the fume hood. The error consisting of time frame is due to the time required for incubation of the treated well plate, and could have derived skewed results. Failure to calibrate the instruments used (mechanical micropipettes) can lead to inconsistent measurement of the solutions added to the wells. Lastly, personal errors could have occured due to the pipettor grazing the cells and resulting in cell death. All of these errors may have led to altered results.
All of the mean values determined by the microplate reader were put into a p-test through the program InStat. Both solutions B and C had a p>0.05 showing that there is no significant difference in cell viability between solutions B and C and the control. However, solution A had a p<0.05 in both datasets, showing that there is a significant difference in cell viability between solution A and the control.
Overall, the data support the hypothesis that if 78 uM, 26 uM, or 8.7 uM aqueous keratin is introduced to muscular tissue, then the cells will not substantially decrease in cell viability compared to the control group. Furthermore, the cells introduced to solution C decreased minimally in viability. However, the cells introduced to more concentrated keratin solutions (A and B) increased in viability. Generally, the data suggest that the addition of aqueous keratin does not negatively affect the cell viability substantially. Through previous research, it was found that keratin does have regenerative, wound healing properties. The data acquired in this investigation suggest that concentrated solutions of aqueous keratin can potentially promote cell growth in vivo.
Discussion: Part Two
Acknowledging that the data suggests aqueous keratin has no foreseen adverse effects on mouse muscle cells, the steps to spin a suture were taken. Through trial and error, various concentrations of PCL, keratin, and glacial acetic acid were created and electrospun onto a copper plate to determine the optimal ratio for a nanofiber.
In Graph 1, the nanofiber with the 60:40 concentration ratio projected the least tensile strength (0.32 MPa) and the least structural integrity, due at least in part to the most beading and fewest thread-like structures, as shown in Image 1. The nanofiber with the 80:20 concentration ratio projected the most tensile strength (3.06 MPa). however the PCL to keratin ratio caused an insufficient amount of keratin to be present in the nanofiber, and, according to Image 3, the strands that formed were thin and fragile. The nanofiber with the 70:30 concentration ratio depicted a tensile strength of 1.32 MPa, and the nanofiber in Image 2 was characterized by evenly distributed and fibrous threads. Qualitatively and quantitatively, the nanofiber spun with the 70:30 PCL to keratin solution suggests optimal concentration for a cardiovascular suture.
While the 70:30 concentration showed promising results on the copper plate, the nanofiber was still lacking sufficient tensile strength. Thus, the same concentration (70:30) was spun onto a makeshift rotating drum which has previously been observed to align and create uniformity within the fibers. Two factors were tested on the rotating drum to see which would improve the distribution of the threads in the fibers: syringe flow rate in mL/hr and rotational velocity in rpm. Decreased flow rate (2.5 -> 2 mL/hr) and increased rotational velocity (400 -> 1500 rpm) increased the tensile strength of the 70:30 ratio fiber as seen in Table 5 from 1.90 MPa to 2.11 MPa. The optimal fiber spun in this study occurred with a syringe flow rate of 2 mL/hr and a rotational velocity of 1500 rpm.
The fibers in Images 6 and 7 are sections of the optimal fiber shown in Image 5 after the degradation test was implemented in two different environments. Images 6 and 7 both demonstrated visual signs of degradation because both fibers appear to have lost their structural integrity. The fiber stored in the incubator became deformed whereas the fiber stored at room temperature became tenuous as it thinned out. The incubator was used to replicate body-like conditions with a temperature of 35°C and the fiber degraded more in that environment. This suggests that the spun keratin nanofiber and potential suture can be considered absorbable when in the human body. Having an absorbable suture for cardiovascular surgery is paramount, because re-entry to remove sutures causes additional risk due to the need for an additional surgery; it is safer to allow the sutures to dissolve over time.
The nanofibers spun were roughly sheets with dimensions 3 cm x 3 cm. To form them into filamentous sutures, the fibers will likely be rolled tightly, but this method will be explored in future studies. Further testing with higher rotational velocities and lower syringe flow rates will be conducted to increase tensile strength. Additionally, a long-term study to see how the suture loses strength over time would be an extension to this study.
Current suture materials used for cardiovascular repair consist of basic materials which were developed many years ago (Rubin, 2016). Through the research conducted in this paper, an optimal absorbable keratin suture was composed using a 70:30 concentration of PCL/glacial acetic acid solution and keratin. This solution was electrospun onto a makeshift rotating drum at varying syringe flow rates and rotational velocities. After multiple tests, a flow rate of 2 mL/hr and rotational velocity of 1500 rpm produced an optimal keratin suture that had a tensile strength of 2.11 MPa, comparable with current sutures being used in the cardiovascular field which have tensile strengths averaging 2.37±0.33 MPa (Karabulut, 2010). The keratin suture has better healing potential than current sutures because it is composed of a protein already present in the body, thus preventing infection post-surgery without compromising suture strength. In other words, keratin has a lower chance of invoking a detrimental immune response. With results that support the proposed hypothesis, this innovative suture material can potentially improve cardiovascular patient recovery time post-surgery.